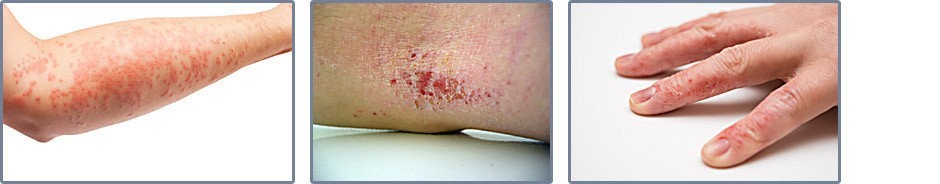
Atopic Dermatitis
Atopic Dermatitis (AD), oftentimes called Eczema, is a very common skin disease. Dermatology Associates offers treatment for children, teens, and adults.
Children often get AD during their first year of life. If a child gets AD during this time, dry and scaly patches appear on the skin. These patches often appear on the scalp, forehead, and face. These patches are very common on the cheeks. No matter where it appears, AD is often very itchy. People may rub their skin against bedding or carpeting to relieve the itch. In children of all ages, the itch can be so intense that a child cannot sleep. Scratching can lead to a skin infection.
Because AD can be long lasting, it is important to learn how to take care of the skin. Treatment and good skin care can alleviate much of the discomfort.
Atopic dermatitis (AD) looks different in infants, children, and adults. The following gives you the signs and symptoms for each age group.
Infants
AD can begin early. A child may be 2 or 3 months old when AD begins. When AD begins early, it often causes:
— A rash that appears suddenly
— scaly, itchy dry skin
— trouble sleeping
— skin infections, commonly due to rubbing and scratchingIt forms on the scalp and face, especially on the cheeks (can appear on other areas of the body), and:
— can bubble up, then ooze and weep fluid
— causes itching that may come and go
— is intensified by rubbing against bedding, carpeting, and other things in order to scratch the itch.Parents often worry that their baby is getting AD in the diaper area. Babies rarely get AD in their diaper area. The skin stays too moist for AD.
Children
When AD begins between 2 years of age and puberty, the child often has these signs and symptoms:
— A rash that often begins in the creases of the elbows or knees.
— Itchy, scaly patches where the rash appeared.
— Other common locations are the neck, wrists, ankles and creases between the buttocks and legs.In time, the skin with AD can:
— Get bumpy, looking like permanent goose bumps
— Lighten (or darken) where AD appears
— Thicken, turning leathery to protect itself from constant scratching
— Develop knots (only on the thickened skin)
— Itch all the time (only on the thickened skin)The thickened skin can itch even when the AD is not flaring. When talking about the thickened skin, your dermatologist may use the word lichenification. This word means thickened skin.
Adults
When an adult has atopic dermatitis, it often looks different from the AD of childhood. For adults, AD often:
— Appears in the creases of the elbows or knees and nape of neck
— Covers much of the body
— Can be especially noticeable on the neck and face
— Can be especially bad around the eyes
— Causes very dry skin
— Causes non-stop itching
— Causes scaly skin – more scaly than in infants and children
— Leads to skin infectionsIf a person has had AD as a child, as and adult may have
— Extremely dry skin
— Skin that is easily irritated
— Hand eczema
— Eye problems (eczema on eyelids, cataracts)Who gets atopic dermatitis?
Around the world, between 10% and 20% of children have AD. About 1% to 3% of adults have AD. People of all skin colors get AD. AD is much more common today that it was 30 years ago. Dermatologists are not sure why. They do know that some children have a greater risk of getting AD.
The following seem to increase a child’s risk of getting AD:
— Family members that have AD, asthma, or hay fever: Does the child’s mother or father have AD? Does a parent have asthma or hay fever? A family history of these diseases remains the strongest risk factor. If one or both parents have AD or an allergic condition, the child is much more likely to get AD. Some children get all 3 diseases. Asthma and hay fever usually appear before the age of 30. People often have asthma and hay fever for life.
— Where the child lives: Living in a developed country, city (especially one with higher levels of pollution), or a cold climate sees to increase the risk. For example, Jamaican children living in London are twice as likely develop AD as those who live in Jamaica.
— Gender: Females are slightly more likely than males to get AD.
— Mother’s age when child is born: When the mother gives birth to the child later in her childbearing years, a child is more likely to get AD.
— Social class: AD seems more common in higher social classes.
What causes atopic dermatitis?
Researchers are still studying what causes AD. Through their studies, they have learned that AD:
— Is not contagious: There is no need to worry about catching it or giving it to someone.
— Runs in families: People who get AD usually have family members who have AD, asthma, or hay fever. This means that genes play a role in causing AD. Children are more likely to develop AD if one or both parents have AD, asthma, or hay fever. About half (50%) of the people with severe AD (covers a large area of the body or is very troublesome) will get asthma and about one-third (66%) will get hay fever.
Can certain foods cause atopic dermatitis?
Foods do not cause AD. But some studies suggest that food allergies can make AD worse. Children who have AD often have food allergies to these foods – milk and foods that contain mild (e.g., yogurt and cheese), nuts, and shellfish.
Before you stop feeding your child any foods, talk about this with your child’s dermatologist. Children need certain foods to grow and develop normally.
Researchers continue to study what causes this complex disease. They believe that many things interact to cause AD. These things include our genes, where we live, and the way our immune system works.
Are the shots that treat hay fever and other allergies useful?
Allergy shots have not proven helpful for AD. Shots may even make AD worse. There is an exception. If the shots treat a patient’s lung allergies, the skin may get better. Before trying allergy shots, be sure to talk with a dermatologist.
topMost children’s AD does not have a clear cause, such as an allergy, but most AD will improve with good skin care. These tips from dermatologists can reduce the severity and frequency of your child’s flare-ups.
Bathing Tips
— Bathe your child in warm – not hot – water.
— Limit your child’s time in the bath to 5 or 10 minutes.
— Use cleanser only when needed and make sure the cleanser is mild and fragrance-free. Do not use bubble bath. If your child’s AD is frequently infected, twice-weekly a diluted bleach bath may be beneficial. Discuss this option with your child’s dermatologist.
— After bathing, gently pat your child’s skin partially dry.
— If your child has medicine that you apply to the skin, apply medicine when your child’s skin is almost dry and use the medicine as directed.
— Apply moisturizer on top of the medicine and to the rest of your child’s skin.Tips for choosing a moisturizer
— When selecting a moisturizer, consider choosing a thick cream or ointment. — — Some children do better with fragrance-free products, so consider petroleum jelly – an inexpensive, fragrance-free product that works well for many children.
— When selecting a product, “trial and error” sampling of different types may help to identify the best moisturizer for your child.Skin care tips
— For best results, apply moisturizer at least twice a day. This prevents dryness and cracking. It also can decrease the need for eczema medications.
— If your child has severe itching and scratching, ask your child’s dermatologist about wet wrap therapy. This can reduce swelling and lessen the desire to scratch.
— Keep your child’s fingernails short and smooth. This decreases the likelihood that scratching will puncture the skin. Putting cotton gloves on your child’s hand at night may help prevent scratching during sleep.
— Keep temperature and humidity levels comfortable. Avoid situations in which the air is extremely dry or where your child may sweat and overheat. This is the most common trigger of the itch/scratch cycle.Clothes-washing tips
— Using a laundry detergent made for sensitive skin may be beneficial. Scented fabric softener or dryer sheets may contribute to irritation.
— Only use the recommended amount of detergent.
— Use enough water for adequate rinsing.
— Buy clothes without tags because tags can rub against the skin, causing irritation.
— Wash your child’s new clothes before wearing. This will remove excess dyes and fabric finishers, which can irritate the skin.Good skin care is a key part of gaining control of your child’s eczema. If skin care has not been a regular part of your child’s treatment, you should make an appointment for your child to see a dermatologist.
top