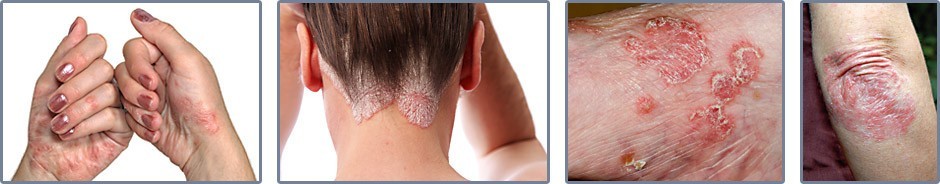
Psoriasis Treatment
Psoriasis (sore-EYE-ah-sis) is a chronic (long lasting) disease. However, knowledge and proper Psoriasis treatment by a dermatologist can provide relief for sufferers.
Psoriasis develops when a person’s immune system sends faulty signals that tell skin cells to grow too quickly. New skin cells form in days rather than weeks. The body does not shed these excess skin cells. The skin cells pile up on the surface of the skin, causing patches of psoriasis to appear.
You cannot get psoriasis from touching someone who has it. To get psoriasis, a person must inherit the genes that cause it.
Types of Psoriasis
If you have psoriasis, you will have one or more of these types:
• Plaque (also called psoriasis vulgaris)
• Guttate
• Inverse (also called flexural psoriasis or intertriginous psoriasis)
• Pustular
• Erythrodermic (also called exfoliative psoriasis)
Some people get more than one type. Sometimes a person gets one type of psoriasis, and then the type of psoriasis changes. You can find out more about these types under the “Signs and Symptoms” tab, below.
What you see and feel depends on the type of psoriasis you have. You may have just a few of the signs and symptoms listed below, or you may have many.
Plaque Psoriasis
(also called psoriasis vulgaris)
• Raised reddish patches on the skin called plaque (plak)
• Patches may be covered with a silvery-white coating, which dermatologists call scale
• Patches can appear anywhere on the skin
• Most patches appear on the knees, elbows, lower back, and scalp
• Patches can itch
• Scratching the itchy patches often causes the patches to thicken
• Patches vary in size and can appear as separate patches or join together to cover a large area
• Nail problems – pits in the nails, crumbling nail, nail falls offGuttate Psoriasis
• Small, red spots (usually on the trunk, arms, and legs but can appear on the scalp, face and ears).
• Spots can show up all over the skin
• Spots often appear after an illness, especially strep throat
• Spots may clear up in a few weeks or months without treatment
• Spots may appear were the person had plaque psoriasisPustular Psoriasis
• Skin red, swollen, and dotted with pus-filled bumps
• Bumps usually appear only on the palms and soles
• Soreness and pain where the bumps appear
• Pus-filled bumps will dry, and leave behind brown dots and/or scale on the skinWhen pus-filled bumps cover the body, the person also may have:
• Bright-red skin
• Been feeling sick and exhausted
• Fever
• Chills
• Severe itching
• Rapid pulse
• Loss of appetite
• Muscle weaknessInverse Psoriasis
(also called flexural psoriasis or intertriginous psoriasis)
• Smooth red patches of skin that look raw
• Patches only develop where skin touches skin, such as the armpits, around the groin, genitals, and buttocks. Women can develop a red, raw patch under their breasts.
• Skin feels very sore where inverse psoriasis appearsErythrodermic Psoriasis
(also called exfoliative psoriasis)
• Skin looks like it is burned
• Most (or all) of the skin on the body turns bright red
• Body cannot maintain its normal temperature of 98.6 F. Person gets very hot or very cold
• Heart beats too fast
• Intense itching
• Intense painIf it looks like a person has erythrodermic psoriasis, get the person to a hospital right away. The person’s life may be in danger.
People who get psoriasis usually have one or more person(s) in their family who has psoriasis. Not everyone who has a family with psoriasis will get psoriasis. But psoriasis is common. In the United States, about 7.5 million people have psoriasis. Most people, about 80%, have plaque psoriasis.
Psoriasis can begin at any age. Most people get psoriasis between 15-30 years of age. By age 40, most people who will get psoriasis, about 75%, have psoriasis. Another common time for psoriasis to begin is between 50 and 60 years of age.
Whites get psoriasis more often than other races.
Infants and young children are more likely to get inverse psoriasis and guttate psoriasis.
Scientists are still trying to learn everything that happens inside the body to cause psoriasis. We know that psoriasis is not contagious.
You cannot get psoriasis from swimming in the same pool or having sex.
Scientists have learned that a person’s immune system and genes play important roles. It seems that many genes must interact to cause psoriasis.
Scientists also know that not everyone who inherits the genes for psoriasis will get psoriasis. It seems that a person must inherit the “right” mix of genes. Then the person must be exposed to a trigger.
Many people say that their psoriasis began after they experienced once of these common psoriasis triggers:
• A stressful event
• Strep throat
• Taking certain medicines, such as lithium or medicine to prevent malaria
• Cold, dry weather
• A cut, scratch or bad sunburnPsoriasis is a long-lasting disease. Here are some things you can do that will help you take control.
Learn about psoriasis. Knowledge really is power. Learning about psoriasis will help you manage the disease, make informed decisions about how you treat psoriasis, and avoid things that can make psoriasis worse. It will also help you talk about psoriasis with others.
Take good care of yourself. Eating a healthy diet, exercising, not smoking, and drinking very little alcohol will help. Smoking, drinking and being overweight makes psoriasis worse. These also can make treatment less effective. People who have psoriasis also have an increased risk for developing heart disease, diabetes, and other diseases, so taking good care of yourself is essential.
Be aware of your joints. If your joints feel stiff and sore, especially when you wake up, see a dermatologist. Stiff or sore joints can be the first sign of psoriatic (sore-EE-at-ic) arthritis. Between 10% and 30% of people who get psoriasis, get this type of arthritis. Treatment is essential. This type of arthritis can eat away the joints. Treatment can prevent deformed joints and disability.
Notice your nails. If your nails begin to pull away from the nail bed or develop pitting, ridges, or a yellowish-orange color, see a dermatologist. These are signs of psoriatic arthritis.
Pay attention to your mood. If you feel depressed, you may want to join a psoriasis support group or see a mental health professional. Depression, anxiety, and suicidal behavior are more common in people who have psoriasis. Getting help is not a sign of weakness.
Learn about treatment for psoriasis. Some people choose not to treat psoriasis, but it is important to know your options. This will help you make an informed decision and feel in control.
Tell your dermatologist if you cannot afford the medicine. You may be eligible for financial assistance.
Talk with your dermatologist before you stop taking medicine for psoriasis. Immediately stopping a medicine for psoriasis can have serious consequences. It can cause one type of psoriasis to turn into another more serious type of psoriasis. Let’s say a person who has plaque psoriasis takes a medicine called methotrexate. If the person just stops taking methotrexate, this can cause the plaque psoriasis to turn into guttate psoriasis or erythrodermic psoriasis. This can be very serious.